|
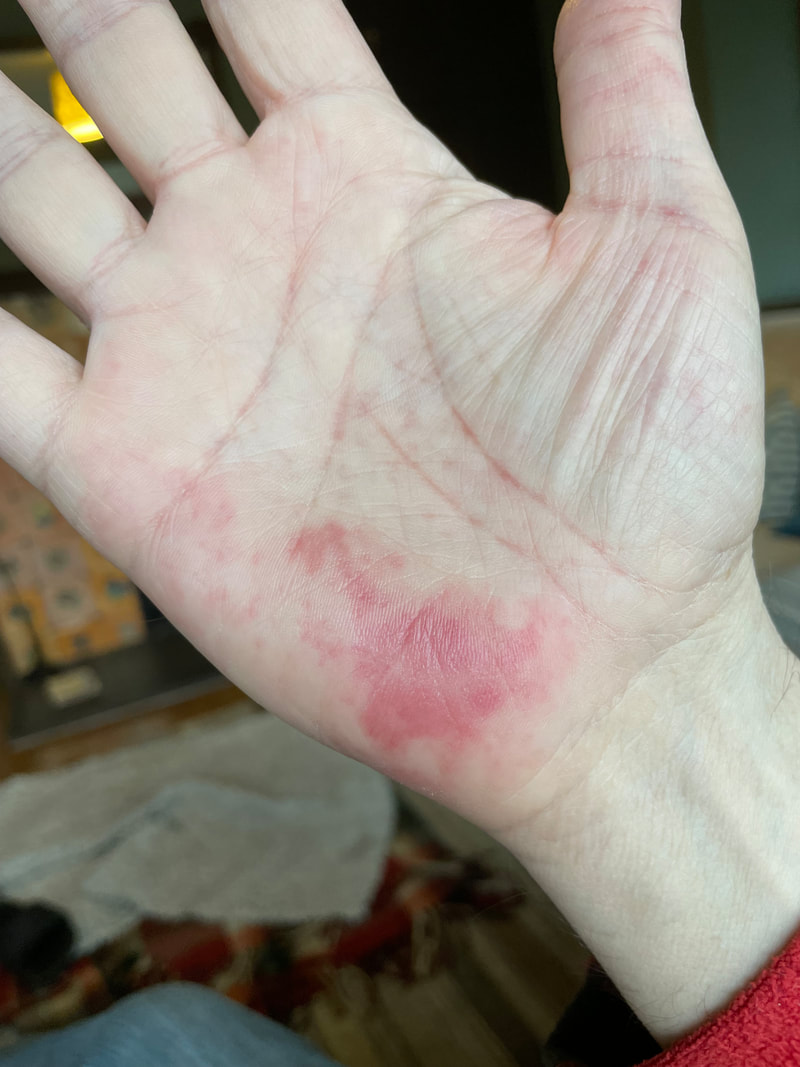
I was diagnosed with MDS a year ago to the day – life looks rather different now. The monoclonal antibody infusion seems to have sorted out the EBV debris left by Amanda. She still hasn’t apologised. The graft versus host disease, GVHD is still active but less so. My palmar rash is under control. My liver function tests are almost back to normal, and I no longer need twice weekly infusions of anti-fungal medicine. Instead I just take 3 mahoosive tablets a day that are hard to swallow. Swallowing is still a big issue, but better than it was. Gums still a bit white. Taste still not right. Whenever I eat, small mucoceles pop up on my soft palate. 2-3mm in size and feel prickly like you’ve got a pip or seed lodged. A bit painful, but then settle and gone a few hours later. Combined with not feeling hungry, and the pain on swallowing, I haven’t been drinking enough. The registrar in clinic 2 weeks back told me my kidney function was worse and I needed to drink more. No problem, I said, but I just kept on drinking 2 glasses of pink milk a day. Then last week the results were worse. Apparently, I was in “AKI” – acute kidney injury (urea 10, creatinine 140). I hadn’t told the family as, unlike my bone marrow, I have 100% faith in my kidneys. They just need to put their big boy pants on and filter a bit harder. Unfortunately, the specialist nurse rang up and spoke to my partner last week and then I was in Big Trouble. What next? Don’t know. Plan is to slowly reduce the steroids, then if GVHD sort of OK, slowly reduce the CyA. Then at some point, another bone marrow, various blood tests, and then when off the CyA I can start having monthly COVID vaccines. Thankfully Boris has defeated COVID for us, but it’s looking unlikely I’ll be able to return to work in June. Hopefully the team can manage without me a little longer...but it’s going to be touch and go for them I fear. GVHD rash on my palms. Basically it's just Mx Donor cells having a bit of fun. Nice to meet you, and thanks for re-building my immune system but can you just leave my mouth and hands alone please? There’s a danger following my last blog, that I could veer into autobiographical story telling …could be dangerous.... I’m usually quite private and can only share this openly because it’s just words on a computer screen, and you can’t see me. Also, you don’t know it’s me because I’ve used a clever nom de plume. You think it’s me, but really, is it?
[Insert sad face emoji] I really miss work. I miss the buzz, the excitement and challenges, the sense of camaraderie when the sh!t hits the fan; speaking to parents, working out best management for the babies and always making the right decision (that’s what INTJs do). I miss morning meetings, chatting with the trainees, coffee with my buddy, lunch with colleagues. [more emojis] I miss getting called in at night – genuinely. Appearing at 2am to intubate a baby plays to the hero complex EVERY doctor has, whether they admit it, or not. Most of all I miss the banter with the nurses. For most of my time at medical school I wanted to be a paediatrician. My first SHO job was in paediatric oncology. I spent my 1-week summer holiday prior to starting, reading a paediatric oncology handbook. Probably a waste of time. On my first day we were taught how to access a Hickman line in case a child presented with sepsis. The Hickman lines were the same as the one that still dangles out of my chest now. Weird. I still remember the faces, names and diagnoses of some of the children who I looked after and died, who I tried to make smile by licking the tip of my nose whilst I took blood. Being ill has really made me think about what it must have been like for the kids and their families. Initially I had no interest in being a neonatologist. I thought most neonatal consultants were probably autistic, unable to cope with children. Might still be true I suppose. The main attraction of a career in paediatrics to me seemed to be the opportunity for mucking around, more banter, not wearing a white coat and avoiding all the pomposity you see in adult specialties. Honestly, if we no longer see patients without wearing scrubs or shirt sleeves rolled up, why do they park their Porsche in the car park, and then ponce around the hospital in 3-piece pin-striped suits and shiny brogues? Aren’t M&S cotton-nylon-mix beige slacks good enough for them? I loved neonates as soon as I first started but was too embarrassed to tell my best buddy because we had already agreed that neonatology was for the emotionally retarded and we were above that. I poo’d my pants the first few days and nights. It was terrifying, but we were immersed immediately. I worked a 1:3 for 6 months. I’m still friends with my two buddies from those times, 30 years ago, one now a PICU consultant, the other an adult ICU consultant and me in NICU. All bases covered. This involved 24 hours on, 24 hours off and then …. a week of 9-5 days and then a Whole Weekend Free. I felt like a key part of the team, I think that’s often lost these days. Very quickly you got good at practical skills. If you messed up the veins, your mate coming on next only had one person to blame. The middle-grade doctor didn’t sleep in, if you didn’t learn to intubate, it didn't turn out well. The nurses, as I’ve said before, look after you, save your bacon and pick you up when you fall. But you’ve got to be nice. Without them, you are toast. I’ve been watching ‘This is going to hurt’ on the TV. Many surgical consultants were like that in the early 1990s. I worked for several arrogant pompous twats, but I also remember many amazing, inspiring and caring consultants. Edmund Hey inspired me to become a neonatologist. His introvert, analytical brain fascinated me. He was creative and innovative, but worked excessively and obsessively, and his family suffered because of that. Those that didn’t know or work for him couldn’t understand why he was so adored. To those that knew, he was a genius. His legacy in terms of clinical practice, academia or inspiration for trainees is unrivalled. Ed died unexpectedly in 2009 and I wept. I still have the email he sent me the evening before he was found dead, encouraging me to do some research study. I still don’t understand why he had such an impact on me, but he was inspirational. It is now 365 days since I worked in the ‘intensive care area’ of NICU. That’s the place I want to be. I enjoy the other areas and research but caring for sick babies and families is where my heart is. I don’t think I’ll ever get back to that now, and it feels sad. 365 days ago, I went to do the job I love, prepared to work the night, but instead came home at teatime with a touch of cancer. At medical school we had lectures on psychiatry but I didn’t pay much attention. But I do remember the very first lecture. Kurt Schapiro walked into the lecture theatre quietly as we were all loudly chatting and nobody initially noticed him. A short, bald man, wearing a black university gown, just standing quietly behind the lectern. As we all slowly saw him, the lecture theatre fell silent. And he just stood there slowly turning his head as he peered over half-rimmed spectacles looking at us. Felt a bit weird. And then, [cue strong German accent] he said, “I suppose by now most of you have realised, that life isn’t fair”. And that is the only thing in psychiatry I ever learned, but it has stayed with me forever. Life isn’t fair. Not for sick babies, their parents, kids dying of cancer, refugees, Ukrainians ... Life isn’t fair, but it’s been fairer to me than most, even now.
34 Comments
|
Authorstart from August 2021 Archives
May 2022
Categories |
 RSS Feed
RSS Feed
