|
It's been 3 months since I last blogged and frankly I've not got much to say for myself. I suppose that's good news. The daily handful of medicines is slowly getting smaller. I still go for the ECP 'Disco lights for lymphocytes' treatment every 2 weeks - always a few regulars on the ward to dance with. I've done some podcasts with charities on 'emotional' topics such as breastmilk donation after baby loss, Trisomy 18/13 as well as the Butterfly project, joined some charities as medical advisor, done work with the WHO and am in process of setting up a charity providing funds for QI projects in Africa. That's enough #virtuesignalling . Written a couple of grants, attended numerous project meetings, webinars, a few papers ... even boring myself now. Basically, it turns out that I still love all things neonatal and am still angry (and sad) that NICU was ripped from me 18 months ago. Worried that I might be too out of touch for the acute ITU work so looking for a role on my return that mainly involves me stroking a grey beard and throwing out random comments. It's all feeling rather autumnal and reminds me of this time last year, end of summer holidays, everyone heading back to school or Uni, and me counting the days until I got admitted for my transplant. I was desperate to avoid getting COVID and keeping my fingers crossed that my donor was being equally careful. Looking back I didn't feel especially scared or anxious, but I was very uncertain how it would feel, and how it would turn out. I started making lists of things I would take in with me - exercise bikes, activities ... when in the end, I spent 80% of my time staring at a blank wall. Every time I did something or said goodbye to someone there was a bit of me that wondered whether that was the last time I might do or say that. Especially felt really bad for my family & close friends as if it was somehow my fault. I'm planning to return to work in late October sometime; have had 2 x COVID vaccines but need a 3rd as I'm immunocompromised. Endless Catch22 of trying to book through a system that isn't set up for the complexities post BMT. I'll get 3rd COVID vaccine along with flu vaccine and all my childhood vaccines again (as all that immune memory has gone now) so will have endless sore arms. Going to need supply of "I've been brave stickers". Oral GVHD does funny things - chronic inflammation leading to fibrosis. Still hoping that might get better over time but it might not. Still can't stick my tongue out, or twist it over or do that curling up thing that I used to impress the kids on paediatric wards with or the nurses on a night out. My swallowing is also not right - can't swallow a large mouthful and certain tablets still get stuck. For what it's worth, GVHD seems to have similar constellation of symptoms to Sjogrens. Systemic chronic inflammatory process might also explain why I still get tired. For the 6-8 months prior to transplant I was anaemic - normal response to this is to increase iron absorption. Coupled with the few blood transfusions I received has meant that my liver got iron overloaded. Normal ferritin (measure of iron stores) is around 25-250 whereas mine was 3000. High levels of ferritin eventually damage the liver. Once iron is in your liver you can't get it out except by making red cells that require lots of iron - so every time I get ECP they also venesect me 500mLs. When they stop the ECP I have locally-farmed leeches lined up. I pulled the corner of a finger nail the other day and licked the blood - it didn't taste nice and felt a little odd, as it's not really mine. I used to be O NEG and I've changed to O POS. I'm not sure that explains the difference in taste. I often catch myself staring at the redness of my palms and thinking that the blood came from someone else's stem cells. I've often thought whether I would choose to find out who my donor was (only if they agreed) and what I might do. Whether I would want to meet them and what I would feel. Can't dwell on that for now, still some way to go. I think many around me imagine I'm almost through it now and want to celebrate. I don't feel like that in the slightest and actually have little interest in seeing most people. Don't take it personally! Silver liningsFortunately there are a few silver linings
I stopped working nights on call when I was first diagnosed because basically it's not possible to jump out of bed at 2am to intubate when you keep fainting with anemia. I won't be going back. I felt a little guilty about my colleagues picking up the extra nights until I calculated that I've done over 5 years of nights since I qualified, almost always working the next day (and often the preceding day) as well. Even if my colleagues pick up 'my' extra nights until I retire they still won't do as many so I've given up feeling guilty. The idea of only working a 40 hour week... I'd had rather disgusting fungal toe nails on big toes for about 10 years. The posaconazole anti-fungal drug I've been on to prevent me dying of systemic Aspergillus infection has done a great job and I now have normal toe nails again. In fairness, the posaconazole for 10 months alone has cost the NHS >£20,000, but still ... The daily steroids have also given me back my 6-pack. Pictures below. I'm having to back off a little now. I've had some grey hair for several years now, but the chemo seems to have destroyed most of my grey hair follicles - like the Tories it presumably attacks the weakest first. Cyclosporin also can make you a little hairy and more curly, so as the hair came back in it seems much less grey and bushier. I'm calling this "peak hair". It may not last.
7 Comments
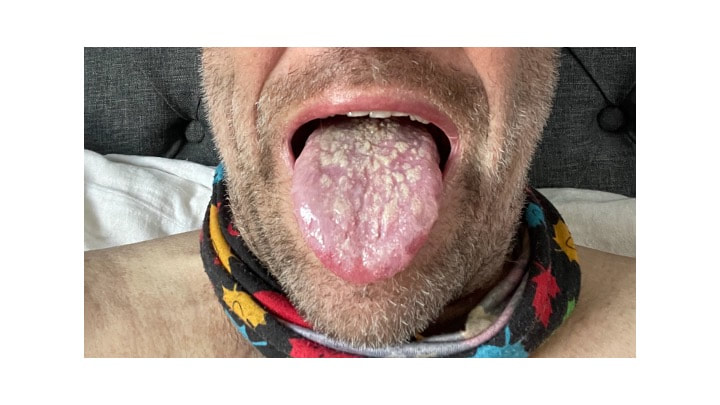
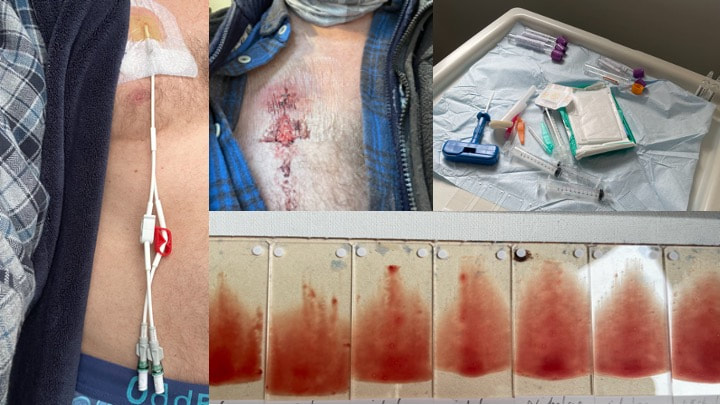
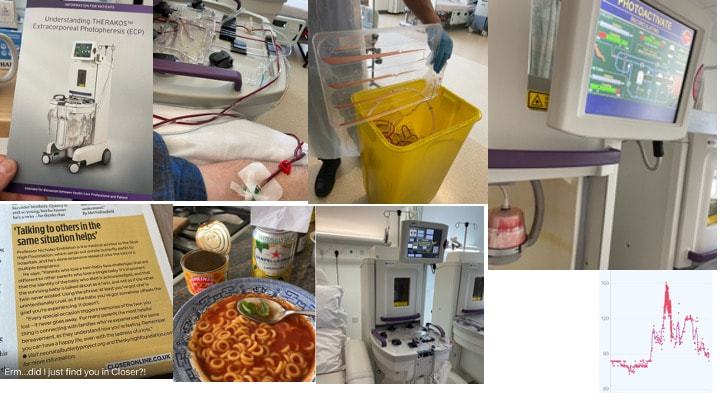
Long delay since my last blog. Read on, no disasters. Trigger alert - photos of blood and bad language. I struggle with writing stuff down, partly because I think it’s a bit boring for others now, but I do get asked how I’m doing so I figure maybe I should write another blog page. For a long while every day was ground hog day. Where did I get to? I had my transplant in October, I didn’t die from septicaemia and my blood counts all started to come back fine. November I was exhausted, but by December I had more energy, walking more using a cunning disguise of sunglasses and masks which probably only served to draw more attention to myself in Newcastle mid-winter. New Year’s Day I started falling apart with graft versus host disease, GVHD, when the new donor T cells started attacking my mouth and liver. Felt dreadful for most of January, started getting a bit better and steroids were amazing. Most of February though I was still on soup and yoghurt. Amanda Trollope’s virus came and teased my B lymphocytes. Still no apology. Even though I felt better in March I wasn’t really on solids as my mouth was still a sewer. Then my excessive swilling of oral steroids resulted in the inevitable oral candida. Nystatin did nothing, nor did Fluconazole. I remained on Posaconazole which is a super expensive oral anti-fungal with activity against almost everything. But with a suppressed immune system you can’t shift candida. If it gets hold that’s it and explains why it’s so serious for preterm babies (and others with dodgy immune systems) once it ‘gets in’. Every morning I look at my tongue trying to work out if it looks a little less disgusting. It does look better in last week or two but it’s still there. I’ve tried scraping it off. With some gentle scraping you can generate a bit of yoghurty froth. But you can’t detach the hyphae which are firmly attached. I don’t want to rub too hard and push the fungus into me. I’m guessing this picture is making it less likely Amanda will ever snog me again. Her loss. Over the last few weeks my steroids have been slowly decreased. Really slow 1mg decrease every two weeks. But I’m now down to 11mg. This has mainly been achieved by starting a new treatment, I’ll get to that in a bit. I had my Hickman line taken out 3 weeks ago so no longer is there anything dangling out my chest and waking me at night. Procedure was OK and I had a nice chat with the registrar as he first just pulled it. Tied string to the end, then to the door handle and a big hard slam but to no avail. Some local injected and then a nice sharp scalpel alongside it taking care not to slice into it because my right atrium blood would just empty onto the bed. After the incision you then do “blunt dissection” with forceps and no sharp metal. Slightly weird feeling having forceps poked in and them some furtling, but if you didn’t know what was happening and you didn’t look it would be fine. Then another bone marrow biopsy. I took a photo this time of it – the blue handled object in the photo below. Need a handle to get a good bit of purchase. Just like a corkscrew. Good firm push and then some sucking. Best not to watch. Still smarts a little. Bone marrow looks OK I'm told, working well, no rogue elements to be seen for now. Obviously quite a way to go, but I’ll take that for now. GVHD can go on forever, but I’ll take a cacky mouth and itchy rashes over being dead. New treatment is called Extracorporeal Photopheresis (ECP). I get it for 2 days every 2 weeks. Decent sized cannula in your elbow out of which a machine takes some blood - maybe 150mL. Nothing to feel but with a cannula in your elbow you can’t bend your arm so I can’t email or write when I’m on the machine. But this is then an excellent time to do PhD supervision sessions and project meetings. I blur the background. But if I feel my heroism hasn’t been sufficiently acknowledged, I might turn my video off, slightly tilt my laptop so you could see the machine, and then turn my video back on without the blur until everyone has seen said machine and then I apologise and pretend I forgot to blur and so on. The 150mL of blood goes into a centrifuge where it gets spun around. This leave red cells at the bottom, plasma at the top and a small layer (Buffy coat) in the middle where most of your white cells are. This is put to one side, the 148mL goes back into you, and then whole process is repeated. After several cycles of that, the few mls of white cells are then mixed with a psoralen which makes the white cells more sensitive to light and UVA light is shone at them (all inside the machine, nothing to really see). The combination of being spun around and made to feel really dizzy, and then given a phototherapy sun tan makes the lymphocytes more chilled about life and they become less pro-inflammatory. Same thing happens the next day. For a few days after I felt a bit tired, but my mouth is better over last few weeks. I’m now being weaned from stage 1 foods onto lumpy solids, and it feels great. I feed myself. Still a bit of choking and pain on swallowing but I can drink coffee again, still can’t do bread or anything ‘meaty’ and most fresh veg still tastes like mud. I can manage chocolate eclairs, chou pastry, crème caramel and I’m finally putting weight on again. Basically, if you can put cream on it I can eat it.
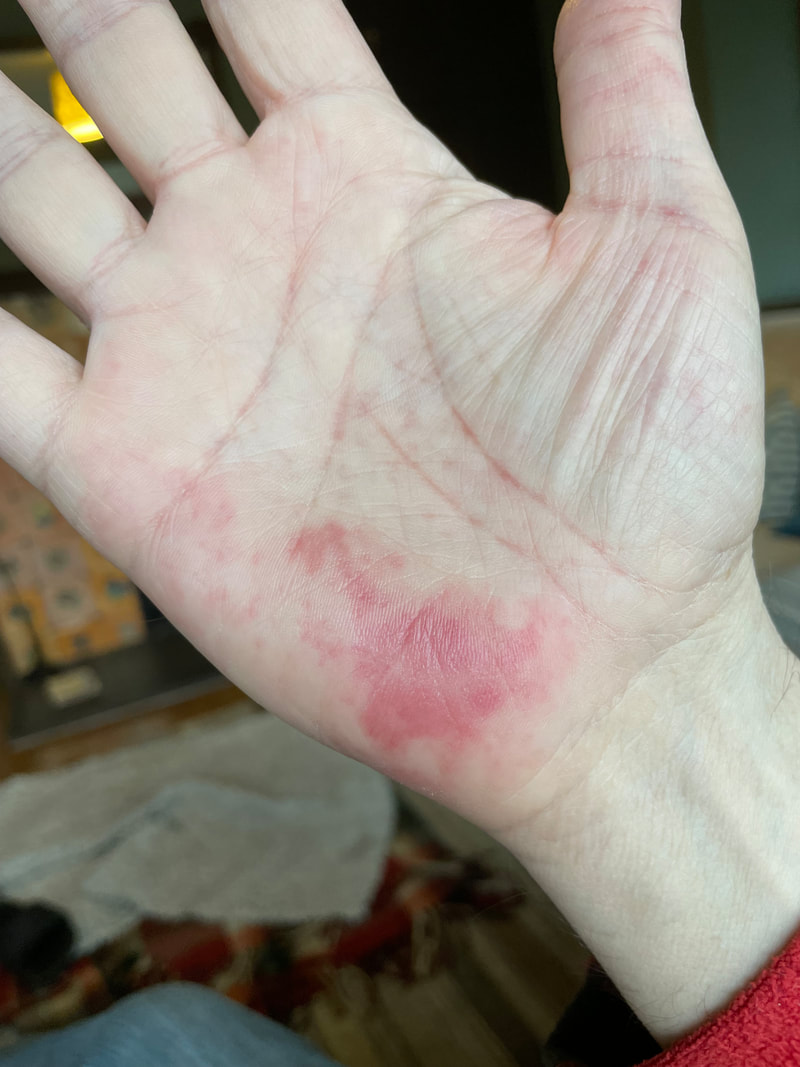
Also, some academic success. Getting a paper in a medical journal like New England Journal of Medicine, is often seen as the pinnacle of many research careers but very few people ever read those sorts of magazines. Unlike Closer. Massive readership, high impact, top drawer. Sadly, it was in relation to Georgina and Cristiano’s loss of a co-twin and our Butterfly project, but media has a short attention span and you get the message out when you can. That’s probably enough for now. I was diagnosed with MDS a year ago to the day – life looks rather different now. The monoclonal antibody infusion seems to have sorted out the EBV debris left by Amanda. She still hasn’t apologised. The graft versus host disease, GVHD is still active but less so. My palmar rash is under control. My liver function tests are almost back to normal, and I no longer need twice weekly infusions of anti-fungal medicine. Instead I just take 3 mahoosive tablets a day that are hard to swallow. Swallowing is still a big issue, but better than it was. Gums still a bit white. Taste still not right. Whenever I eat, small mucoceles pop up on my soft palate. 2-3mm in size and feel prickly like you’ve got a pip or seed lodged. A bit painful, but then settle and gone a few hours later. Combined with not feeling hungry, and the pain on swallowing, I haven’t been drinking enough. The registrar in clinic 2 weeks back told me my kidney function was worse and I needed to drink more. No problem, I said, but I just kept on drinking 2 glasses of pink milk a day. Then last week the results were worse. Apparently, I was in “AKI” – acute kidney injury (urea 10, creatinine 140). I hadn’t told the family as, unlike my bone marrow, I have 100% faith in my kidneys. They just need to put their big boy pants on and filter a bit harder. Unfortunately, the specialist nurse rang up and spoke to my partner last week and then I was in Big Trouble. What next? Don’t know. Plan is to slowly reduce the steroids, then if GVHD sort of OK, slowly reduce the CyA. Then at some point, another bone marrow, various blood tests, and then when off the CyA I can start having monthly COVID vaccines. Thankfully Boris has defeated COVID for us, but it’s looking unlikely I’ll be able to return to work in June. Hopefully the team can manage without me a little longer...but it’s going to be touch and go for them I fear. GVHD rash on my palms. Basically it's just Mx Donor cells having a bit of fun. Nice to meet you, and thanks for re-building my immune system but can you just leave my mouth and hands alone please? There’s a danger following my last blog, that I could veer into autobiographical story telling …could be dangerous.... I’m usually quite private and can only share this openly because it’s just words on a computer screen, and you can’t see me. Also, you don’t know it’s me because I’ve used a clever nom de plume. You think it’s me, but really, is it?
[Insert sad face emoji] I really miss work. I miss the buzz, the excitement and challenges, the sense of camaraderie when the sh!t hits the fan; speaking to parents, working out best management for the babies and always making the right decision (that’s what INTJs do). I miss morning meetings, chatting with the trainees, coffee with my buddy, lunch with colleagues. [more emojis] I miss getting called in at night – genuinely. Appearing at 2am to intubate a baby plays to the hero complex EVERY doctor has, whether they admit it, or not. Most of all I miss the banter with the nurses. For most of my time at medical school I wanted to be a paediatrician. My first SHO job was in paediatric oncology. I spent my 1-week summer holiday prior to starting, reading a paediatric oncology handbook. Probably a waste of time. On my first day we were taught how to access a Hickman line in case a child presented with sepsis. The Hickman lines were the same as the one that still dangles out of my chest now. Weird. I still remember the faces, names and diagnoses of some of the children who I looked after and died, who I tried to make smile by licking the tip of my nose whilst I took blood. Being ill has really made me think about what it must have been like for the kids and their families. Initially I had no interest in being a neonatologist. I thought most neonatal consultants were probably autistic, unable to cope with children. Might still be true I suppose. The main attraction of a career in paediatrics to me seemed to be the opportunity for mucking around, more banter, not wearing a white coat and avoiding all the pomposity you see in adult specialties. Honestly, if we no longer see patients without wearing scrubs or shirt sleeves rolled up, why do they park their Porsche in the car park, and then ponce around the hospital in 3-piece pin-striped suits and shiny brogues? Aren’t M&S cotton-nylon-mix beige slacks good enough for them? I loved neonates as soon as I first started but was too embarrassed to tell my best buddy because we had already agreed that neonatology was for the emotionally retarded and we were above that. I poo’d my pants the first few days and nights. It was terrifying, but we were immersed immediately. I worked a 1:3 for 6 months. I’m still friends with my two buddies from those times, 30 years ago, one now a PICU consultant, the other an adult ICU consultant and me in NICU. All bases covered. This involved 24 hours on, 24 hours off and then …. a week of 9-5 days and then a Whole Weekend Free. I felt like a key part of the team, I think that’s often lost these days. Very quickly you got good at practical skills. If you messed up the veins, your mate coming on next only had one person to blame. The middle-grade doctor didn’t sleep in, if you didn’t learn to intubate, it didn't turn out well. The nurses, as I’ve said before, look after you, save your bacon and pick you up when you fall. But you’ve got to be nice. Without them, you are toast. I’ve been watching ‘This is going to hurt’ on the TV. Many surgical consultants were like that in the early 1990s. I worked for several arrogant pompous twats, but I also remember many amazing, inspiring and caring consultants. Edmund Hey inspired me to become a neonatologist. His introvert, analytical brain fascinated me. He was creative and innovative, but worked excessively and obsessively, and his family suffered because of that. Those that didn’t know or work for him couldn’t understand why he was so adored. To those that knew, he was a genius. His legacy in terms of clinical practice, academia or inspiration for trainees is unrivalled. Ed died unexpectedly in 2009 and I wept. I still have the email he sent me the evening before he was found dead, encouraging me to do some research study. I still don’t understand why he had such an impact on me, but he was inspirational. It is now 365 days since I worked in the ‘intensive care area’ of NICU. That’s the place I want to be. I enjoy the other areas and research but caring for sick babies and families is where my heart is. I don’t think I’ll ever get back to that now, and it feels sad. 365 days ago, I went to do the job I love, prepared to work the night, but instead came home at teatime with a touch of cancer. At medical school we had lectures on psychiatry but I didn’t pay much attention. But I do remember the very first lecture. Kurt Schapiro walked into the lecture theatre quietly as we were all loudly chatting and nobody initially noticed him. A short, bald man, wearing a black university gown, just standing quietly behind the lectern. As we all slowly saw him, the lecture theatre fell silent. And he just stood there slowly turning his head as he peered over half-rimmed spectacles looking at us. Felt a bit weird. And then, [cue strong German accent] he said, “I suppose by now most of you have realised, that life isn’t fair”. And that is the only thing in psychiatry I ever learned, but it has stayed with me forever. Life isn’t fair. Not for sick babies, their parents, kids dying of cancer, refugees, Ukrainians ... Life isn’t fair, but it’s been fairer to me than most, even now. What's going on? The graft versus host disease (GVHD) is still rumbling but less than it was, although the initial response to a higher dose of cyclosporine didn't boost energy or mouth much so I was started on some steroids (prednisolone 30mg OD) just over a week ago which were .... amazing! The day after the first dose I was able to get out of bed with a spring, less aching, more positivity, got my work brain on and started emailing and catching up on projects. Mid-January I had no desire to leave the house, but in the last few days I have started walking around the park again. My gums are back to pink, but my palate is still sore, inflamed and covered in red spots and tiny cysts, and swallowing medicines is uncomfortable. Rashes are settling but everything still tastes pretty gross, a bit like chewing sandpaper and mud, so I survive on yoghurt, porridge, tinned fruit, energy drinks and pink milk. My mouth also gets pretty dry so I've been given some saliva in a squirt bottle. They tell me it's not donated. I've got some hair on my head, makes life much warmer. New hair is baby soft so I spend plenty of time gently stroking it. Don't judge me, you would too if you could. I had thought January was going to be relatively straightforward and the big news would be the repeat bone marrow biopsy looking for the extent of any residual disease ... but this is going to be topsy turvy so that biopsy is 'on hold' for now. My oral GVHD meant I dropped out of lots of zooms and other meetings I had wanted to do. A friend had given me great advice "to be kind to myself" so I dropped out without feeling my usual guilt of letting people down. But I have been able to join a few meetings and speak, especially on the Butterfly course we released a few months ago. I might blog on that another time but if you want to do the course it's completely free, just lick the link. It means a lot to me that people see it. If you've been paying attention, you'll remember that the BMT gave me a whole new blood AND a whole new (but naive) immune system. All your white cells (neutrophils, lymphocytes etc.) and the antibodies you produce ultimately start in your BM so a transplant resets your immune system back to the beginning. Whilst I'm making red blood cells and platelets and white cells fine, the white cells are troublesome. These new lymphocytes see my body as 'foreign' and try to reject me. Stupid really, if they just stopped to think they'd realise that was an act of mutually assured destruction. The cyclosporine keeps my 'new' immune system under control whilst we learn to be friends. But a consequence of this is that I am "immunosuppressed" - and my usual ability to keep infections under control is limited. It's basically walking a tightrope between infection and getting rejected. Bit like what Amanda did to me. Whilst many of these infections are just lurking around the environment or on passers by, we all carry viruses that hang around in our body forever. These are particularly the herpes family of viruses that reactivate, usually after a bit of stress. Cold sores are herpes that lurk in your nerves and reactivate when you're feeling sad, have to write an essay or stay 10 minutes late after work. Shingles is your chickenpox virus coming back years later. CMV can very occasionally reactivate during pregnancy with devastating consequences for the foetus. Epstein Barr Virus (EBV) gives you glandular fever as a teenager but almost never reactivates in later life, although traces of EBV hang around in the cells at the back of your mouth and throat and your B lymphocytes forever. Risk of viral reactivation post-BMT is well known, so some drugs I take (acyclovir, letermovir) are used prophylactically to prevent some of these, but there isn't an anti-viral for EBV in this way. The level of EBV can be measured on bloods and you could find low numbers in lots of people but 10-20,000 copies is high and 60,000 is getting pretty high. Mine has gone from 6,000 to 9,000 to 32,000 in just 10 days, so I was admitted as a day case a couple of days ago for treatment using a monoclonal antibody (artificially synthesised) which you would expect would directly target the EBV, but in fact targets the B lymphocyte cells that carry it. This is because the real risk here is not infection as such, but what the virus does to B cells. The EBV in the B cells makes them all frisky and they go on a mad one. Un-checked this can lead to a lymphoproliferative disorder, a bit like a lymphoma which is really not good news. The monoclonal antibody is called Ritoximab which has a list of side effects which includes basically anything you can think of, including other virus reactivation (because you're killing off some of your immune system.) Trying to understand what is going on without a medical degree would be pretty complex. Anyhow, it's all been fine so far and the £££ cost, like Stella Artois, is reassuringly expensive so it must be good. Someone needs to take responsibility here. Unlike the MDS which I am happy to put down to bad luck, I most certainly know who is responsible for this clusterfuck of immunological complexity and she's called Amanda. It was the heady summer of 1979. Sony had produced the first Walkman, the 3-mile nuclear accident threatened disaster, and Maggie came to power but I was fully distracted by getting a girl friend. Stuart Hutchinson had gone out with Amanda previously and told me she was 'playful' so I set off on my mission. There was going to be a 'pyjama party' at a friends house in a couple of weeks (life was pretty racey back then) so I needed to make a pre-emptive move fearing I wouldn't be able to compete for her attentions when there were more players on the market. In the late 1970s, cinema's largely existed for teenagers to snog in, and James Bond's Moonraker film was just released (the one with jaws in it). 90 pence each for a ticket was quite steep, especially as you hope you're not going to see much of the film, but she agreed to come along, and we sat in the back row. I'm pleased to report Stuart's inside info was as accurate as Sue Gray's report will be. Party time indeed.
Sadly, a few days later I started feeling quite unwell, nasty tonsillitis and a trip to the GP confirmed I had glandular fever caused by EBV. Amanda had taken the playfulness too far but there was no going back. Not only was I poorly and feeling crap, I couldn't go the pyjama party. I was gutted. She didn't even ring to apologise. She went to the pyjama party where she copped off with Thomas Alcock who bloody fancied himself but I thought he was a twat. He was from the year above and bigger than me, so any thoughts of revenge were put to one side. Bollocks to both of them. Suffering the double rejection of my new graft and Amanda is making this a particularly difficult time for me. I've literally no idea what is going to happen next. The plan is to try and wean both the cyclosporine and steroids bit by bit, spend some more of your taxes on expensive drugs, and do more blood tests. Right, enough chatting, pass the saliva. Not going to lie, the start of 2022 has been crap. Things had all been going well, and I was slowly reducing my cyclosporine (CyA). Remember, this is a commonly used immunosuppressive drug that keeps lymphocytes (a type of white cell) under control and is used in most people following a transplant. However, its use following a BMT is unlike use in 'solid organ transplants'. After any organ transplant, your body's immune system will recognise that donor organ as 'foreign' and try and destroy it. This results in inflammation that if left untreated, would slowly result in damage and failure of the new organ, be it kidney or heart etc. That is because your lymphocytes will always recognise it as foreign, so you need to stay on CyA (or similar) forever. If you start to get rejection, then it can be treated by increasing the dose of CyA or adding in new drugs like steroids. This is why getting a well 'matched' donor is important whether it is bone marrow or kidney. Better matches result in less rejection or inflammation. The situation following BMT is almost the opposite of this. In this case, the new donor bone marrow (graft) starts to produce lymphocytes that are initially kept under control by the CyA. This keeps your lymphocyte numbers low, but it also means you are at slightly higher risk of infection (because you are suppressing your immune system). Infections that are particularly problematic are viruses like herpes or CMV, but also more unusual infections like fungus or weird things that used to be seen in people who are HIV+. When you are taking lots of CyA you also won't respond to vaccines very well, so you have to wait to get your COVID vaccine until you are ideally off CyA or on low dose. Over time, the CyA dose is decreased - that started early December and was going OK. However, just after Boxing Day, I first started feeling tired, a bit achey like flu, and then my lips started tingling before becoming a bit painful. I also developed some mild liver inflammation and my CyA dose was increased. Unfortunately, there's a lag time between increasing the CyA and suppressing the lymphocyte activity and within 2-3 days I had developed a really sore mouth. My lips lost their outer layer, turned bright red and swelled. It looked like I'd had collagen fillers. Then the whole of my mouth developed white plaques that slowly coalesced and my gums turned white. They're still white now although the ulcers are settling. Basically, the new donor lymphocytes went on a mad one and turned my mouth into a sewer. They've had a massive party in my mouth without permission AND failed to tidy the mess. The graft was attacking me (host) hence the term GVHD. I was going to take a photo, but even I was grossed out looking at my mouth. My taste buds that had been recovering have taken a beating, and just about every food except for milk and yoghurt tastes disgusting again. I also developed a widespread itchy rash over chest and back, and a very painful purple rash with tiny cysts on my palms. Fortunately I don't have it on the soles of my feet - if I did it would make walking extremely painful. Steroid creams and steroid mouthwashes +++ and good mouthwash to keep it all clean. The tiredness and exhaustion is crippling, not sure why it's so bad, but at its worse, I could hardly sleep; consequently I have done nothing useful for 2 weeks now. That's really irritating me. Not even played the piano.
What next? Not really sure. Important to get this episode of GVHD under control - whilst I can cope with rashes, and my mouth will settle, I don't like the idea of something important like my liver getting hit. We've increased the CyA twice now so I am on the same dose as when first discharged but will need to try and decrease again when things are under control. I've gone from loathing CyA to thinking of it as my temporary saviour! Chronic GVHD is not uncommon, but hopefully if that happens it won't be as severe as this episode. I'm optimistic it will get sorted out, but GVHD can obviously be pretty serious. I'm always looking for silver linings otherwise all of this would be relentlessly depressing, but there is some good news. It means the graft is working well - thanks Mx Donor, I still love you even though you're trying to kill me. I'm sure we can reach a compromise. Also, a strong graft has a slightly better chance of being a strong cuckoo and ousting those malignant host bone marrow stem cells. Slightly less likely for the graft to fail. Still, long way to go, slowly slowly. Rather than share a picture of my mouth, here's a random photo of me biting my brother. I don't seem to be able to do regular blogs. My INTJ brain thinks about writing an update, then over-thinks why it will be rubbish, and fairly quickly gets distracted by something more interesting. Then, I start getting messages from people wondering how I'm getting on, perhaps concerned that my lack of blogging is a sign that all is not well. Well, OK, things are "fine". Still on my usual cocktail of drugs - CyA, Acyclovir, Letermovir, Septrin, magnesium, vitamin D - but the CyA dose will now start to decrease as we are T+65 days or thereabouts. I'll explain about CyA, lymphocyte counts & immunity in the next post; bit bored of that for now to be honest. Blood counts all stable - Hb 116g/L, WCC 3.16, Plts 175, Neutrophils 1.99, Lymphocytes 0.63. My Hickman line is still in-situ and working fine, still gets in the way when I sleep. Occasionally, the dressing pulls on what little chest hair I have left (it was basically a rug prior to chemo) and wakes me up in a cold sweat as my dreams turn to nightmares about it getting pulled out by accident and me dying in a pool of blood as my right atrium empties itself in my bed. If you were asleep, how would you ever know you were slowly bleeding out? Apologies to anyone else with a Hickman ... don't worry I'm sure this can't really happen. This blog post really goes on and on for ages, so feel free to skim. But I need to write "as one". In summary I live a blissful life for about 50+ years convincing myself I am bullet proof and will live to 100 before I get told I've a serious bone marrow problem, get a bit upset and struggle to find the right time to tell anyone. The next few paragraphs just milk it a bit, but that's the gist. I've not written that much about getting the diagnosis previously but the events of that day will be scarred in my brain forever. You'll remember that I had been feeling tired for a few weeks, but hadn't considered anything was actually 'wrong'. Just thought I was un-fit, or had spent too much time indoors over the COVID winter. My family kept telling me I looked pale, but that made no sense to me as I had no reason to be anemic. There's only two ways to really lose blood - gut or urine - and I was 100% sure I hadn't lost blood. I couldn't be anaemic - I was eating fine, and getting all the iron, B12 etc. you might need, so to my brain it was impossible that I might be anaemic. In an earlier post, I explained how I told a GP friend that it felt as if I was unable to "off-load" oxygen to my muscles and wondered if I could have long COVID - without actually having had COVID. If I'd sat with a doctor, even a medical student, who'd took a half decent history, they might have twigged fairly quickly that I had a bone marrow problem. Looking back after I was diagnosed, I remembered that in early January when I had my 2nd Pfizer Covid vaccine, that I had ended up with a 1cm bruise at the injection site. It was a perfectly round bruise and I just assumed a bigger blood vessel than normal had been pranged. About a week later, I developed a whole load of petechiae (tiny pinprick haemorrhages under the skin due to low platelets) on my forearm - caused by the shoulder strap of a heavy rucksack as it slid down my arm when I took it off. They were very distinct and I knew that they didn't mean anything as they were localised just to an obvious site of skin trauma, and weren't anywhere else. They disappeared over the next hour or two and I forgot about them. I only remember these facts in retrospect. By chance the week before I was diagnosed, as I was starting to think I should get my bloods checked because of the tiredness, I got an 'out of the blue' email from my GP telling me to book in for routine bloods. I didn't know GPs did routine bloods like that but it all seemed quite convenient and made myself an appointment for the following week on Thursday. Two days before diagnosis, I spent the Sunday afternoon cleaning my bike. Mainly because I was still convinced there was an obvious reason for feeling tired when cycling uphill - the most likely culprit (rather than cardiovascular physiology) was that there had been a build up of grit and dirt on my chain. I spent a good 2 hours sorting my bike out and polishing my gears and chain. I can remembering thinking 'that will sort it'. I'm squirming as I'm writing, about how after 30 years of medicine I could miss such an obvious explanation to my tiredness. Don't judge me too harshly. Sunday night. Lying in bed, on my side, reading my kindle and I realise that for the last couple of nights I've had to "re-arrange" myself to get comfortable. I didn't have any pain, or discomfort, but I lay on my back and gave myself a good examination. I didn't have any obvious lumps but I couldn't feel my testicle on the right side as I had what I was fairly sure was a hydrocele. A hydrocele is basically a collection of fluid around the testicle that can be a sign of infection, tumours etc. but equally might be nothing. Testicular cancer tends to present before 50 years age, but can be painless and just cause a hydrocoele. There's nothing embarrassing about a hydrocele or swollen testicles. Monday. When I woke and showered I realised my right testicle was possibly a little sore, and decided I should get examined. I had a day of webinars and meetings that were obviously far too important to cancel, and decided I would simply go to A&E first thing Tuesday morning. I knew I would need an ultrasound scan at least, and I could get my bloods done at the same time. I know I should have seen my GP first, but going straight to the hospital (where I worked) seemed more time efficient for everyone, especially me. Tuesday. I'm rostered to be on call tonight on the NICU, so don't cycle to work as normal, as I take the car when on call at night in case I need to return urgently. Go to my office, say a quick hello to colleagues and immediately go to A&E which is almost empty. Present myself to the nurse sitting at the triage desk who seems a bit irritated with my arrival. "Yes" she says abruptly, beckoning me forward. "What's wrong?". "I've got a hydrocele" I say in what felt like a fairly matter-of-fact tone. "What makes you think that?" she replies, slightly sarcastically I think. "Because I'm a doctor" I reply. She raises her eyebrows, clearly irritated that [yet again] it's just a middle aged bloke complaining about his scrotum and not a true emergency. "Alright, check in at that desk there." She didn't apply to work in A&E to deal with those sorts of minor genital irritations. Now, the fact that I'm a doctor doesn't really explain why I thought I had a hydrocele but it seemed the simplest explanation. I took a seat, dialled in to zoom for the NICU team handover meeting, waited an hour whilst nothing happened in A&E - zero patients, zero activity - and just as I was about to pull rank to go and tell the medics to finish their tea and toast, a junior medic took me into a room. Full examination, bloods, ECG - agreed I had a hydrocele and needed an ultrasound. I waited 2 hours (I'd taken my laptop & rucksack knowing waiting was likely so busied myself sorting emails), but radiology was really busy, and I was told it'd be simplest if I could make my way to the hospital on the other side of town for a scan. The medic offered to organise a taxi to take me there, but I remembered I had my car (as I was due to be on call in 6 hours time). Just before I walked out the door, I asked the medic if any of the blood results were back. "I've only got the ferritin back, but it's raised" he said. Seemed odd to me, a full blood count normally gets processed in under an hour but there was no apparent news on my Hb. Ferritin can be a sign of iron-overload or chronic infection. Mine was about 4-5x upper limit of normal. I asked the medic what he thought, and what could possibly connect that sort of ferritin result to a hydrocele that had only been there for a couple of days. "Well, it can be a sign of chronic inflammation he said [yeah, obvs, I am a doctor] and it's possible to get unusual infections, like atypical TB (tuberculosis) in the testicles." I felt more than a little bit irritated with the suggestion that I might have been engaged in dogging sessions with badgers, but alarm bells were starting to ring. I drove across town to the other hospital, get to the car park, realise I don't have any money on me so won't be able to exit the car park when I need to be on call, so drive and park a way away down a back street. Mid-winter, I have no coat (I was supposed to be on a nice warm NICU), arrive on admissions unit shivering, go to the reception desk. Receptionist: "oh, hello Dr Pants, how are you? I used to work on maternity reception, I remember you. Why are you here?". Me [with pride] "the biggest pair of bollocks you've ever seen" in a voice loud enough that all the ward could hear. Actually, I just whispered 'hydrocele' sheepishly behind my mask. Get given a cubicle, asked a series of questions by the admitting nurse, walk of embarrassment down the ward trying not to spill my bowl of steaming p!ss and then get examined by urology medic who agreed an ultrasound was needed. This is now about 3-4 hours after my bloods and I knew the results must be available. Asked the medic and was told "Haematology are looking at your bloods at present, and the haematologist is going to come and chat to you this afternoon." Massive alarm bells. I asked the results so far - Hb 85 and platelets 75. Clearly my bone marrow was seriously ****ed. It was starting to look like I wouldn't be able to work the night on NICU. Ring a colleague, swore them to secrecy, and told them to sort my night out. Medic asks me thoughtfully if I want to call anyone to be with me when the haematologist comes. I decide I can handle this alone for now. Just give me access to google and the blood results and I could do a good impression of adult physicians. Hmm. Whilst waiting for the ultrasound, my medical brain was now busy diagnosing. Could be lymphoma, or leukaemia (less likely) - seemed unlikely. Didn't really feel that sick, had no lymph nodes, lumps or hepato-splenomegaly, night sweats etc. Hydrocele didn't really fit with that diagnosis either. Could be testicular cancer, but if this had already spread and caused this degree of bone marrow failure I was probably incurable. Could it be a small primary tumour somewhere else, that had metastasised to testicle and bone marrow? Finally, get my ultrasound scan, testicles look pretty normal. Impressive, I'd have said, although the sonographer didn't use that actual word. Some hyperaemia (increased blood flow) but nothing much, and a pair of simple hydroceles. No lumps. No cancer. I think I felt just a tiny bit reassured at that stage, and decided I had lymphoma which I knew was treatable having had two friends diagnosed and successfully cured over the last few years. Sh!t happens I decided, but it could be worse. Turns out, it was. More importantly, I'd failed to make the diagnosis before the specialist arrived. That's always a bit irritating. Haematologist again offers me to contact someone else to be with me, I decline. Yet again, they do know better than me. They explain that the blood film also shows some blasts - these are 'primitive' white cells that are pre-leukaemic - and that I'll need a bone marrow biopsy. Likely diagnosis was myelodysplasia and not lymphoma or leukaemia but I don't think I really heard the MDS term straight away. Check my diary, tell the haematologist I can come for my bone marrow tomorrow (surely it would be a day case procedure, and I'd get a short GA and some morphine) but reassured that local anaesthetic will be fine, and they'll do it now. A very calming, experienced haematologist does the bone marrow trephine. Lots of lignocaine but still hurts. We have nice chats about staff we both know having worked locally in the same hospitals for 30 years. Surreal. I tell her about my research. Her eyes don't obviously glaze over. Clearly a professional. Platelets are pretty low, and I can feel the blood trickling down my back. A few tears trickle down my face, but I've still got my mask on so they get absorbed by that before I roll back over and anyone could see I might have got something in my eye. Quickly remember how my daughter tells me that "tears are only weakness leaving the body" so pull myself together and sneak a very quick look at the trolley with various pots of my bloody bone marrow in them. Surreal and deeply unpleasant. Haematologist disappears with what looks like half my bone marrow on a trolley, and I'm alone in the room. Ears ringing. WTF just happened? The nurse returns, gives me my appointment for the next day to get the results in clinic, some antibiotics in case the hydroceles indicate infection (all swabs were negative btw) and I get up and leave saying thank you to the staff and gesticulating to the receptionist that all is fine, just a pair of massive gonads. I can't go home, it's 4pm and I'm supposed to be working the night, so I text the family, tell them I got lucky and someone else needs to work the night for me, and that I'll be home soon. Walk to my car in the mid-winter rain still just wearing my shirt. Not really sure what to do but I remember in the movies that you can bang the steering wheel with your hands and shout f***! So I do that. But not too hard in case I bruise my hands (low platelets, safety first). Really not sure what to do next, but start driving away from the hospital. Somehow, without real planning, I end up in the car park of a small country park, turn the engine off and start sobbing. No tissues, tears and snot all over my cheeks. It's now 4.30pm, getting dark and the park is closing. I suddenly realise I'm surrounded by hundreds of parents with small children looking at this strange man in a car on his own crying. Quickly realise I look like I've committed a terrible crime and just buried the body, so I exit car park and pull up in a housing estate. Again, without any real conscious thought, I get my phone out and record an audio diary. I've listened to the first few seconds again, but not all of it, or the other 10+ hours I've recorded since then. Don't think I'll ever play them or let anyone else ever hear them. I finally get home for supper at a believable time, eat with partner and youngest child pretending everything is normal, and we sit together to watch TV. Probably Vikings. Realise with some sadness that I'll probably never get to be Ragnar Lothbrook now. Desperately want my youngest to go to bed so I can tell my partner. Time's ticking on, the hole in my back from the bone marrow is starting to hurt and soon one of my other children will be getting in from work. I need to tell my partner, but suddenly find myself alone watching TV and decide to quickly google my diagnosis - I'd just recalled it wasn't leukaemia but likely MDS. Get some out-of-date stats from the US that basically say that I've had it, and suddenly I realise my partner's upstairs having a shower getting ready to go to bed. Knowing I have a large and blood-stained dressing on my back that would need explaining, I charge upstairs, brush my teeth, jump into bed before they do, and open my kindle. Partner gets in to bed, also starts reading kindle. I stare at the pages clicking back and forward (to make it look like I'm reading) whilst I work out the best opening line. Think through various phrases and words that convey the seriousness, but also indicate that I'll be fine. I was at the hospital today darling ... [obviously]
Realise with horror that partner has not only finished reading, but is snoring deeply. F***! What to do? Wake them up or tell them in the morning. Decide that morning will be OK. In fact, start thinking I could perhaps go to clinic to get my results, whilst pretending I'd just gone to work again. Try and read more on my iPhone under the duvet. My lack of knowledge and google combine with endless stories of woe into a night of utter desperation and misery. Shed some more tears whilst avoiding any noisy sobbing. Try and listen to a podcast. What would be appropriate for the situation? Basically, I can't sleep, realise I've probably had it, and tell my partner as soon as they wake in the morning. Email my haematologist before clinic to ask that they don't tell my partner just yet that I'm going to die, go to clinic, get the proper diagnosis, realise I'm not about to die but that bone marrow transplantation is on the cards .... and the rest is history. I told you this blog would go on a bit. You didn't have to read it all. This is likely to be a really boring post. Feel free to skip it and wait for a more interesting blog. I've tried and failed every day for the last 10 days to write something, but just couldn't motivate myself to write. Nothing bad has happened. In fact, nothing's happened. Literally nothing. My blood counts are all 'fine'. Hb somewhere around 110g and neutrophils somewhere between 1.7-1.9. My platelets had shot up to 230, but then about a week ago were back down to 95. That might seem alarming but I'm reliably assured that is perfectly normal to have a brief period of over-excitement in a new relationship before settling. 95 is enough.
Main issue is relentless mix of mild exhaustion, mild nausea, and moderate anorexia where most foods smell and taste disgusting, After trying a range of foods I can manage most fruit juice, Coca Cola etc. especially with ice; just about manage hot chocolate (decent energy & protein in the milk but not really a favourite); ice cream; apple pie etc. But anything bread, wheat, meat, cheese or anything with a smell makes me nauseous. On the plus side I've stopped losing weight. Fortisip (300kcal, 18g protein) in 125mls 2-3 times a day definitely helps. I'd mentally prepared myself for feeling tired, and "changes in taste or appetite" but hadn't expected to feel nausea/anorexia and dislike eating this long post transplant and chemo. Now 6 weeks since my chemo, and again I've been reassured that this is normal but after a while it sort of drags you down. and that's mixed in with total lack of motivation to do anything. Literally anything. I even find myself staring at a blank TV screen when a show finishes, wondering if I can be ar$ed to change channels. Obviously endless Netflix & similar that I could watch. Just can't be bothered. I could read medical papers, or watch webinars etc. Just can't be bothered. Still go to clinic twice weekly. Unfortunately nothing truly positive from a disease perspective can come out of those visits. The precise blood counts don't really matter (unless all my neutrophils suddenly disappeared - very unlikely). My cyclosporin levels clearly need careful monitoring and dose adjustment, and could cause some kidney/liver impairment, but again can all be dealt with. Nothing about the visits/bloods are really about monitoring disease progress; it's all about the side effects of the treatment for the disease. With other diseases as things improve (or worsen) you might feel less pain, or have X-rays or scans to check for disease remission etc. If you were a premature baby, you could rightfully see weight gain, coming off ventilation or oxygen as the disease getting better. But until I get a bone marrow at T+100d there's not much to see or feel to show 'progress'. Even at day 100 there's along period of further uncertainty. Of course, I don't really want any excitement before then, and this may all sound like "oh poor me" but it's not. Many others struggle with much bigger challenges. I'm just trying to explain how exhausted and demotivated you can get. Everyone will experience it differently. Personality clearly plays a big role here. I love projects, mainly academic/research or work related, but could be house related etc. There's little point planning projects when I've no idea when or if I'll get to do them. I'm goal orientated but try to tell myself to enjoy the journey getting there. I like "big picture" and get bored with some of the necessary detail. Like following the instructions. If you're always generally right, why would you follow them? A few of you may think that any amateur attempt to group people into 1 of 16 personality types is "Mickey Mouse" psychology, but I first completed a version of this 20 years ago and it definitely opened my eyes to how strange all of you are. You can take the test here - only takes 10 minutes www.16personalities.com . Take the test and see. If you are borderline on 1 or 2 domains it might give a result that doesn't feel quite right, but most people I know tend to agree with the type they are given. Being caring, sensitive, insensitive, self-obsessed, brave, clever, stupid are possible with any personality type. This is not about how you behave in public, this is what motivates you. I am INTJ-A , and there's nothing about this journey I can enjoy, or influence in any way, and suspect my lack of opportunities for projects because of circumstance or energy, contributes to just feeling flat and frustrated. Other personality types will struggle just as much, but in different ways. Took me half of my adult life to realise how different I was compared to others. I simply didn't understand why you weren't all interested in what interested me. When I tried to explain to you, your eyes just glazed over and you told me to get on with the ward round. How could you not be fascinated by those things? If you do the test and want to, share your personality type in a comment or message. But NEVER share it online/Facebook as that's how Cambridge Analytica rigged the US elections and Brexit vote. They worked out how caring, sensitive and easily swayed you are, then targeted posts at you. Fools. Of course, I've just done that here, however, as I'm always right (even if I'm occasionally wrong, which I never am) and can outsmart them all, I have no fear in sharing. As I said, I told you this was going to be a boring blog, and thank you for reading this far, or at least pretending to. The boring bone marrow in the title was also a pathetic and perhaps not particularly funny way of linking in that I had a bone marrow test last week. Purely for research purposes. I might do a separate blog about research, but this was my way of being vaguely heroic for the advancement of science at some (albeit brief) personal cost. I.e. it is still bloody painful as they were sucking it out even though hopefully it all belongs to someone else. And if any of it is still mine, well then it can f*&k off as I don't like you anymore. I felt this was my penance for not donating blood over all those years. Thank you Mx Donor I am very grateful for what you did for me, and thank you to all your heroes who always donated, or have been persuaded to donate blood after reading the blog. As Nike said if you haven't already, 'just fucking do it'. Right, now that I've done that, I can go back to staring at walls. Thanks for listening x I've thought about writing this post for 48 hrs now but somehow couldn't find the energy. But the Big News is that I did get home a couple of days ago after 27 nights. The staff on the ward have been amazing. Caring, efficient, professional; most importantly I really trusted them. Before I went in, I imagined week 1 would be horrific with chemo, week 2 would be anxious and exhausted, week 3 I'd be on the exercise bike, and by week 4 I'd be exercising, answering emails, catching up with zooms. Whereas, even now, I get tired just eating or simply brushing my teeth. Getting home means better sleep, choice of foods. The smell of most foods (even ones I could eat) makes me nauseous and many still taste weird. Fruit juice and ice gets me through the day. I was gutted to find out that Orangina actually has small amounts of grapefruit in it (forbidden if you are on cyclosporin!).
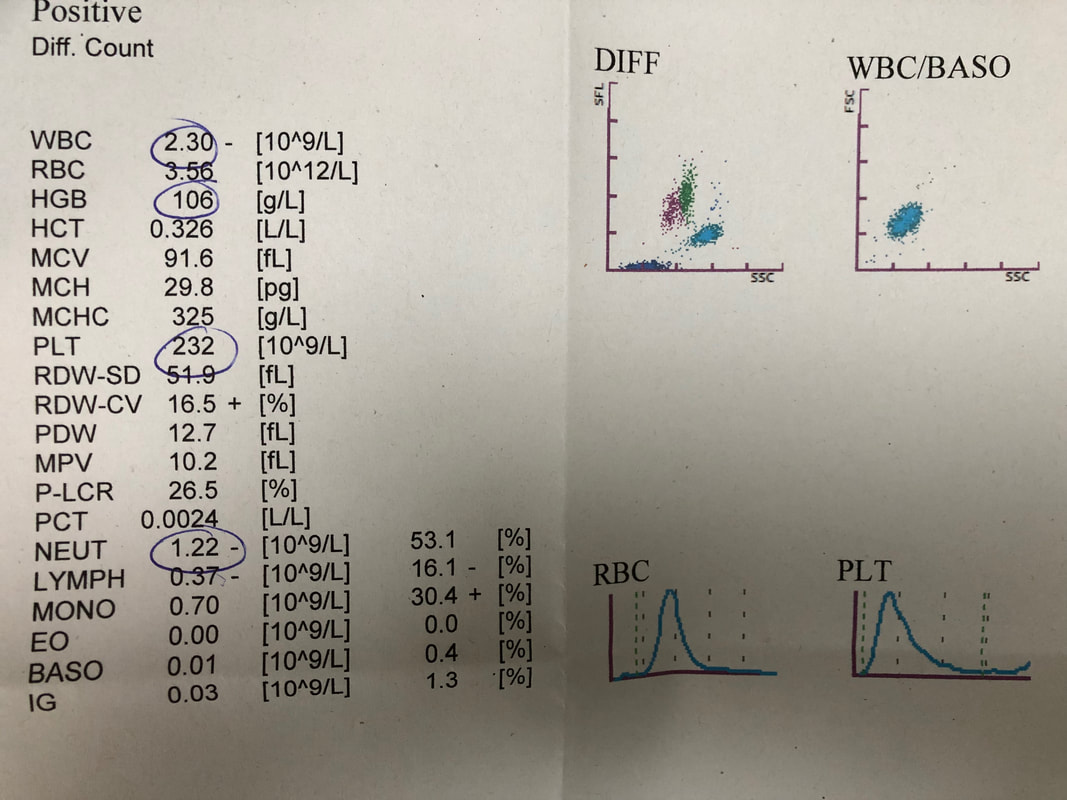
Fortunately, I live close to the hospital, so getting back to clinic yesterday was simple. I have to go twice weekly for bloods, check my Hickman line etc. I still sit in the clinic waiting area trying to work out by looking what other conditions people have. Completely pointless really, as there are no tell tale signs of most haematological disease except extreme pallor and those of us with no hair. Getting to this stage is a good start - I'm now entering the "100 days". At that stage I get another bone marrow biopsy where they look to see the number/proportion of any residual mutated stem cells. Hopefully, the chemo and the cuckoo will have done their job, but it is still possible to have some residual cells at that stage and still get through. But it is the thing I most worry about. Having two cell "lines" is called chimerism - I'll talk more about this another time. And I still need to share my frankly ridiculous behaviour on the horrific 'diagnosis day', telling the kids and 'being brave'. But for now, that's all folks. Oh, btw neutrophils are 1.22, and my platelets are the highest they've been in 2021. Not bad ... Taking a stack of oral tablets every day is a pain, but banana flavour energy drinks - Fortisip - actually help them go down and disguise the taste. Some are really foul. Cyclosporine smells like weed (nurses told me that). Chewable Magnesium is disgusting. But aside from that minor irritation, a bigger problem is smell and taste. I can’t now stand tea or coffee which is quite upsetting as I used to love drinking that. Many other foods also taste different and I’m now really struggling with hospital food, so family bring in an evening meal which makes all the difference. Many foods I can’t stand the smell of – just about any food smell triggers mild nausea, even food I could eat. Lips tingle and mouth feels strange, but thankfully I didn’t get any real mucositis or ulcers. Of course, cyclosporine is the guilty party, I’m sure. As punishment for getting a platelet count >50 (it’s now 111 woop woop!) I get to give myself Tinzaparin injections every day to stave off blood clots.
Slowly getting used to be completely bald, but the only mirror is in bathroom, so I only see myself once/day when I shower. Deeply disturbingly, I seem to look more like my younger brother than me with no hair. When I pull the shower curtain back, I suddenly find he's been watching me. Worse still he’s also naked. Rather alarmingly, the groin swab has grown Pseudomonas. Interestingly, it seemed to start as a small boil with no swelling - remember back when it started, I had no neutrophils so there was no ‘pus’. Many of us on NICU have seen Pseudomonas infecting premature babies, presenting as a rapidly spreading infection up lymph vessels and veins, with areas of black i.e. dead skin. I would guess half those babies die, so this isn’t a bacteria to muck about with, especially when in close proximity to one's genitals. The black spot was also very painful in a way most boils are not. At the time, we discussed with consultant who suggested pseudomonas on basis of black spot, so I knew this was a possibility, and the Tazocin is an appropriate antibiotic. Pseudomonas are clever bacteria - been around longer than we have, and have special ‘efflux pumps’ that push out antibiotics making them highly resistant. They can create biofilms e.g. around Hickman lines, which are almost impossible to treat without removing the line. For some reason, they also grow better in zero gravity: they did an experiment in the space shuttle. Why they did that, and who funded it is a mystery. [Obviously I googled that, but I knew the rest, honest]. I seem to have developed a bit of “chemo brain fog”. Aside from my constant apathy and lack of energy, I’ve found I can’t play more complex pieces on the piano. I can’t seem to read the keys (flats and sharps) and make my fingers play the right notes. I suppose that reading music and playing is a fairly complex cognitive task, and I’m OK on the simple pieces. I’m not ashamed to admit that depressed me quite a bit, but it’s just another thing to work around and I will get better. Still, along with all the other changes, it makes me realise some of what others undergoing more intense chemo must contend with, and I feel so sorry for kids who have to endure all this crap. I was full of bravado when I was first admitted. I thought the first week of chemo would be horrible, the 2nd week would be a bit miserable, but by weeks 3 and 4 I would be up, bed made and ready for kit inspection by 8am, hour of exercise, work, emails, piano, lunch and repeat. The exercise bike was next to my bed for 3 weeks until they took it away. It had been constantly mocking me. You lazy, pyjama-wearing slob, you can’t even bare to look at me. Honestly, I don’t know what I do all day. Time seems to pass quite quickly doing nothing. A few of you wondered why I brought a tape measure in with me. I’ve measured my mid-arm, mid-thigh and abdomen weekly (once a growth and nutrition expert, always a growth expert etc.) The results are in and rather surprising. When I was first told back in April I would need my HSCT in October I asked what I needed to do, and my consultant told me I need to put on some weight. That was deeply irritating given I’d spent lockdown exercising to get down from my porky 74kg to a trimmer 72kg. Most transplant recipients lose <10% body weight, so I ate every pastry going even when I wasn’t hungry and weighed in as a Super Middleweight at 77kg. I’m now around 74kg but forcing myself to eat even when not hungry. My mid-arm circumference has only gone down by 0.5cm. Not much at all. But my mid-thigh has gone from 55cm to 50cm. You might think that is only 10%, but actually it’s more. Circumference is 2*Pi*r and volume is Pi*r2*height, and doing the math, that’s actually a 17% loss of muscle mass. You would also imagine my abdomen had shrunk, using those carefully accrued fat stores. I was 99cm – I had quite a belly – and now my mid-abdomen is…. 99cm. No change. My muscles (lean mass) have slowly atrophied releasing plenty of energy as the amino acids are converted into glucose and fat. That looks to have provided all the extra energy needed, and there's been no need to start burning the fat, although longer term that would happen. It also shows you why BMI, or weight alone, doesn't really tell you the important changes. Losing weight by eating cabbage soup and not exercising is not only pointless, but harmful. Loss of muscle mass results in higher levels of tiredness, muscle weakness and more trips and falls. This is why being bed bound as an older person is a real worry. On the plus side, there's plenty of spaces to launch the dart at for my heparin injection. I didn’t get any bloods checked today, but things are heading in the right direction and yesterday my Hb was up to 90, and neutrophils up to 0.33. Slowly slowly catchy monkey. Once again, thanks for all your comments and wishes, and support. It's good to hear from you even if I don't reply. That's all folks. End of last week and the weekend were largely un-eventful. White counts and platelets stayed down, neutrophil count 0.00 and spent most days lying around watching rubbish TV and snoozing. Somehow, I’ve been in this 4x5m room for 19 nights already. The room is in positive pressure so there’s a constant flow of filtered air into the room which then outflows via gaps around the door. Although the temperature is constant, there’s a continual slight draft, and it feels dry. You wake after a few hours of mouth breathing with cacky mouth and dry lips. Still taking daily showers with Octenisan; showers are deeply un-satisfying, slight draft from the airflow, not quite powerful enough, feel chilly when you get out. I’m not complaining, appreciate how lucky I am to get all this for free. The food is fine, but hard to eat when you never feel hungry, and when you ordered it 24 hours earlier – know I could eat more if I could choose my own food there and then. Force it down best I can, cocktail of tablets for desert; must be eating enough as weight is steady.
Woke up on Sunday morning to realise my hair had suddenly started falling out - bed looked like a dog had been sleeping in it. My jumper changed from cashmere to mohair. One of the nurses shaved it short for me – at that stage I was rocking the Ragnar Lothbrook look with my beard but then that last 1cm fell out, and my beard started disintegrating. Still got the eyebrows but think they’ll go next. Apparently getting your eyebrows plucked out and tattooed back in is all the rage. I think Ragnar does that in series 3. I also realise the last time I had no hair and a naïve immune system was as a newborn baby. It goes without saying that I was beautiful, and back then my immune system was fully supported by breastmilk. Sadly, I now look like an grossly oversize 25 weeker yet I’m no more likely to get breastmilk than I am to get a bed-bath. Have been Octenisan washing, gargling with stuff that tastes like sea water and thought I’d kept it all pretty clean. But Monday I didn’t feel right. Temperature went to 37.6 and I got a sore spot in groin which developed into a shallow ulcer. You don't get 'pus' when you don't have neutrophils. Later on Monday, my temperature hit 38.9, CRP went up to 40, then 59 and I started feeling shivery. Peripheral and Hickman line blood cultures etc. then started back on Antibiotics (Tazocin plus shot of Gent) which is i.v. infusion every 6 hours so they finish at 1am and start again at 6 am. I’ve never had more than 4-5 hours of sleep at a stretch since I arrived. I feel a bit better today, but good news is I HAVE A NEUTROPHIL. You should normally have a neutrophil count of about 3.0 or more, but it could be OK to be a bit lower. Yesterday mine was 0.06 and they have to have come from the donor stem cells. My platelets are also holding up (44) some of which will also be donor. Today my neutrophils are 0.09. Slow but ‘convincing’ I am told. So, thank you Mx Donor; it does feel good. Long, long, way to go and many other future issues to contend with, but for now I’m grateful to get through these first steps. Thank you to all of you for commenting either via social media, on the blog or directly. I’ve been genuinely touched by how many people have contacted or messaged me and apologies if I didn’t respond. I was trying to be consistent and not comment or ‘like’ on social media but I may not always have been consistent! Thank you for all your offers of support. I’ve currently declined all the offers of travel, and most gifts of >£1,000, but I have accepted delivery of this boat. Designed by Stinky Jim Dad Bad Donkey (long story), who also designed the tugs that finally shifted the Ever Given in the Suez. True story. That’s all folks. x |
Authorstart from August 2021 Archives
May 2022
Categories |




 RSS Feed
RSS Feed
